Age-related macular degeneration (AMD), also known as age-related macular dystrophy, is a chronic progressive retinal disease that affects its central part (the macula). This small area is responsible for central vision and visual sharpness, which are essential for reading, recognizing faces, driving, and other daily activities. It is also the area with the highest concentration of light-sensitive cells. AMD is most commonly diagnosed in people over the age of 50 and is one of the leading causes of vision loss in older adults.
Symptoms:
- deterioration of central vision;
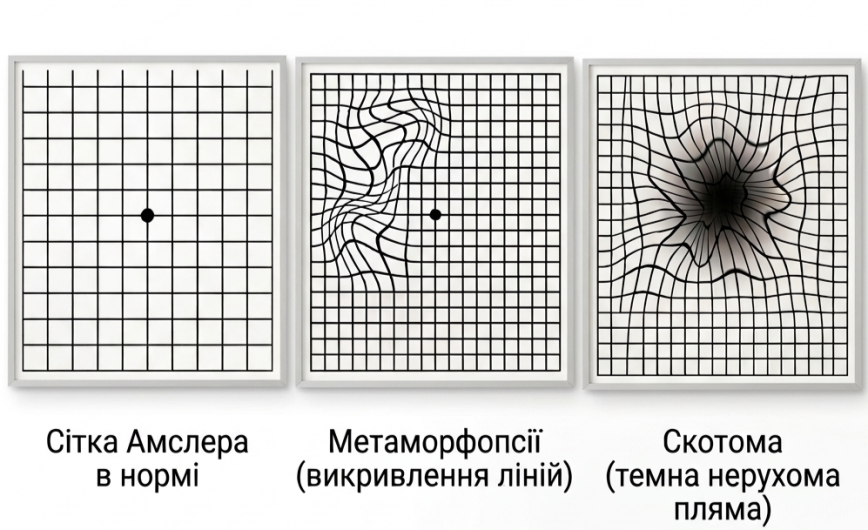
- distortion of straight lines (they may appear wavy);
- dark or semi-transparent stationary spots in the center of vision;
- colors appear less vivid and contrast becomes reduced;
- difficulty reading or recognizing faces;
- reduced contrast sensitivity (poor vision in dim lighting).
This disease is caused not only by the natural aging of cells, but also by other factors:
genetics – having AMD in close relatives increases the risk of developing the disease by 2–4 times;
smoking – increases the risk by 2–3 times and has a strong negative effect on blood vessels;
arterial hypertension, atherosclerosis, and diabetes – impair retinal blood circulation;
ultraviolet radiation – damages the retina;poor nutrition – a lack of antioxidants (vitamins C, E, zinc, lutein, omega-3) weakens retinal cell protection, while excessive intake of saturated fats contributes to deposit formation;
excess body weight – disrupts metabolic processes in the retina;
sedentary lifestyle.
Another important contributing factor is a disruption in the synthesis of vascular endothelial growth factor (VEGF). This is a protein responsible for the formation of new blood vessels. An increased level of VEGF leads to neovascularization — abnormal growth of fragile new vessels that can easily rupture and bleed.
This condition is caused not only by the natural aging of cells, but also by other factors:
| Type | Description | Frequency |
|---|---|---|
| Dry (atrophic, non-exudative) form | It develops slowly, often over many years. Metabolic waste products accumulate in the form of yellowish protein deposits (drusen), and the cells of the macula gradually undergo atrophy. | ~85–90% of cases. |
| Wet (neovascular, exudative) form | Abnormal new blood vessels form beneath the retina. These vessels are fragile, prone to bleeding, and cause swelling. Vision can deteriorate rapidly. | ~10–15% of cases, but accounts for ~90% of vision loss in AMD. |
AMD can only be detected before noticeable vision problems appear through a preventive retinal examination by an ophthalmologist using modern diagnostic methods.
Diagnosis includes:
- fundus examination (ophthalmoscopy / fundus photography);
- OCT (optical coherence tomography) – visualizes the structure of the macula and retina;
- OCT-A (optical coherence tomography angiography) – a non-invasive assessment of retinal blood vessels without the need for dye injection into the bloodstream, as required in fluorescein angiography.
- Amsler grid – a test for detecting distortion of straight lines (can be done at home).
The manifestations of age-related macular degeneration (AMD) depend on its form (dry or wet) and stage of the disease. In the early stages, symptoms may be subtle or unnoticed, but as the condition progresses, clear central vision disturbances appear. The most favorable prognosis is when the disease is detected at an early stage — before vision loss occurs. Therefore, regular eye examinations after the age of 50 are extremely important.
Treatment also differs depending on the form:
| Type | Treatment |
|---|---|
| Dry | Unfortunately, there is no specific cure, but progression can be slowed:
|
| Wet | The most effective treatment method is:
|
When should you get examined?
- patients aged 50+ — mandatory retinal examination every 1–2 years;
- in case of a family history or presence of drusen (yellowish protein deposits under the retina) — annually or more often;
- if there are complaints of image distortion or central visual spots — immediately, even if the symptoms are mild.
Prevention
Lifestyle has a much greater impact on your vision than it may seem at first glance. The best way to combat AMD is to minimize risk factors that we can directly control.
- Smoking cessation — both traditional cigarettes and electronic devices. This is one of the most important factors, as it doubles the risk of developing retinal degeneration.
- UV protection — don’t forget about sunglasses: high-quality UV filters protect the macula from photochemical damage.
- Balanced diet — leafy greens, fatty sea fish (omega-3), colorful fruits and vegetables rich in antioxidants reduce the risk of developing the wet form of AMD by ~30%.
- Monitoring health indicators — high blood pressure and cholesterol damage retinal blood vessels.
- Self-monitoring — use the Amsler grid: it can be placed in a visible area where you can regularly check it. This helps detect early signs of the wet form of AMD.

Kushnir Nataliya
Ophthalmologist, Candidate of Medical Sciences